CREDIT: Center for Drug Evaluation and Research
If you've experienced a change in your prescription drug coverage--don't worry. This happened to me recently and I may be able to help you figure out why this is happening and what you can do about it.
When I went to pharmacy to fill my shampoo prescription for my dermatitis with my new health plan, I found that it had gone from being free to having a small copay. While the new copay was still within my budget, I wanted to know why this was happening. After some similar inquires from our own MomsRising members on why their prescriptions costs have changed, I decided to dig a little deeper. The good news is you have options!
But first things first—Why?
Your health plan, like any private health plan, has a list of prescription drugs they do cover under their plan that are made up of generic and brand name drugs—which is often referred to as the formulary. These drugs are often categorized into 3 Tiers. Tier 1 is made up of the lowest costing generic drugs, Tier 2 is made up of higher costing generic drug formulas that may include brand name ingredients, and Tier 3 is often made up of mostly brand name drugs. In some cases, there is also a Tier 4 designation for specialty, high cost prescriptions. Your prescriptions, even birth control, all fall under one of these tiers.
So great, but what does this all mean?
IMAGE CREDIT to www.kuwaitiful.com
These tiers are important because these designations are what determine if your prescription is free, has a low copay, or has a high copay. And more importantly, your health insurance provider decides what these designations will be.
This means that your insurance company can decide what prescriptions they will or will not cover as long as the drugs on the list meet FDA standards. Formularies can also change often. For example, if you had a brand name prescription with no generic equivalent, it has to be covered and may be designated to a lower tier. But if a generic version of your prescription is added to the list, your current brand name prescription will likely move from a lower tier to a higher tier—resulting in the cost change.
If you find there was a change in your copay or if your prescription looks a bit different, this might mean there was a change on the formulary and you may need to take some steps to get the prescription covered or changed.
Here’s what you can do if your prescription isn’t covered.
If your prescription is no longer covered or if you’ve experienced a copay change, the first thing you should do is ask your insurance company for a list of the prescriptions they cover (the formulary) and what tiers they fall into since it’s possible your prescription moved to a different tier.
Once you have that list, you can talk to your doctor or health provider about possibly changing to a generic version of your drug that is more affordable under the formulary or your doctor can ask for your insurance provider to approve coverage for your current prescription based on their medical recommendations.
If you continue to experience problems having your prescription covered, you can also file for an appeal. It might take some time, but if you work together with your doctor and follow these steps, you should be able to find an affordable prescription that works for you.
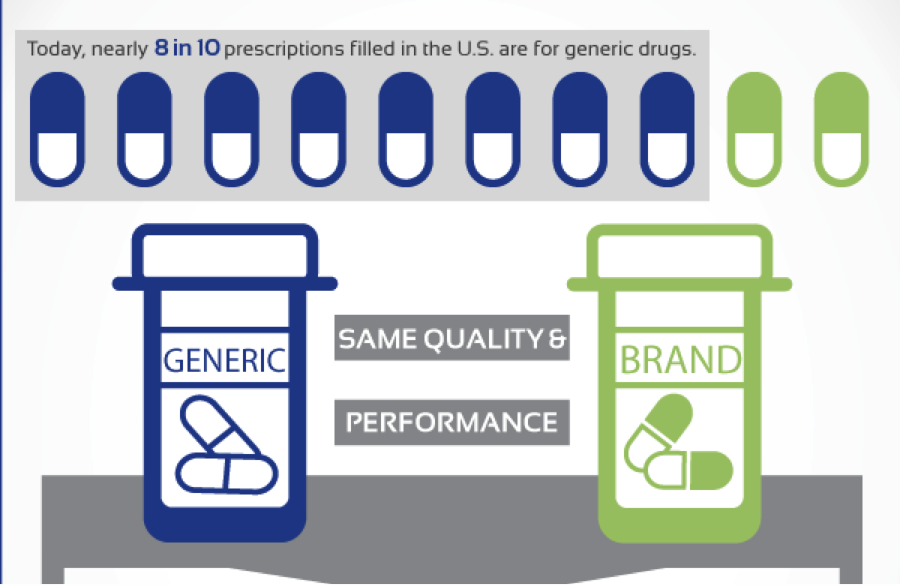
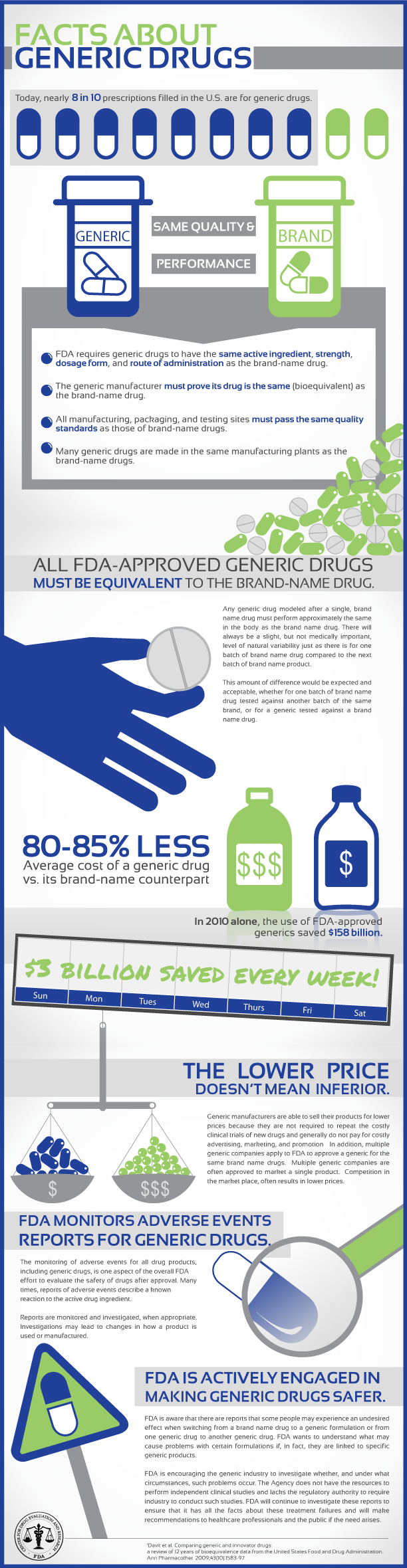
If you feel uneasy about switching from brand name to generic, make sure to talk to your doctor first, but note that the “FDArequires generic drugs to have the same active ingredient, strength, dosage form, and route of administration as the brand name drug” (see the graphic below for more information).
If you still have questions about this or other parts of your new coverage, please don't hesitate to email us at healthbeat@momsrising.org.
IMAGE CREDIT: Center for Drug Evaluation and Research




The views and opinions expressed in this post are those of the author(s) and do not necessarily reflect those of MomsRising.org.
MomsRising.org strongly encourages our readers to post comments in response to blog posts. We value diversity of opinions and perspectives. Our goals for this space are to be educational, thought-provoking, and respectful. So we actively moderate comments and we reserve the right to edit or remove comments that undermine these goals. Thanks!