This morning, for the first time in almost a year, I did not take a pill when I got out of bed. The reason I took these pills, and the reason I stopped, has to do with a word I learned recently:
Iatrogenic, which means 'caused by the doctors.'
I'll start at the beginning.
For six years, I "balanced" a demanding job, a commute, and raising young children. All things considered, I thought I was managing really well until just before my last child turned one year old. Then, the stress and exhaustion I'd been holding at bay engulfed me. I could barely get out of bed, or eat, or think. I couldn't work, so I took a leave of absence.
I made an appointment with a psychiatrist who, naturally enough, prescribed anti-depressants. Makes sense, right? Because by the time I dragged myself into her office, I was really, really depressed.
I was also really, really anxious. I was having horrible, crippling panic attacks almost daily, and I was waking up in the middle of the night, shaking, heart pounding, unable to go back to sleep.
The anti-depressants were supposed to help with this also. Unfortunately, they made me jittery. Now, on top of the anxiety I was already grappling with, I couldn't sit in a chair without jiggling my knee up and down. They gave me other weird side effects: night sweats, headaches, cotton mouth. I started having a lot of trouble sleeping, but it was hard to tell whether it was a side effect of the anti-depressants, since I'd been having trouble sleeping when I was working, too.
So my psychiatrist wrote me a prescription for pills to help me sleep.
Things slowly started to get better for me. Summer came and went. I stopped feeling depressed. I quit my job for good. I started eating like a normal person. But still, I couldn't get a decent night of sleep without taking a sleeping pill.
I quit coffee and chocolate and started doing a lot of yoga and meditation. Still, I couldn't sleep without pills. If I didn't take them, I would wake up between 1 and 3 am, heart pounding, and stare at the ceiling for a good two hours before I could sleep again. After several months of this, I developed an eye twitch.
My psychiatrist, who was intelligent, thorough, and sincere, suggested I do a sleep study. I packed up my pillow, kissed my husband and the kids good night, and drove to a sleep lab in Berkeley. There, a young women with pale skin and dyed black hair skillfully strapped me to various machines designed to monitor breathing, leg movements, brain waves, and God knows what else.
Naturally, I had another terrible night's sleep. Which was sort of good news...
When the results came back a few weeks later, there were pages and pages of detailed findings. There was a problem with my breathing, with my "index of sleep arousals" and with something called RERAs, an intriguing acronym that was never spelled out. In short, I had a "moderate" version of sleep apnea.
My doctor called as soon as she got the results.
"This could be what's causing your depression!" she said. "We need to get you an apnea machine so you can breathe at night. Katrina, if this works, then all your problems may vanish!" She was triumphant. I was hopeful.
Back I went to my HMO. A respiratory nurse named Joan patiently outfitted me in the latest artificial breathing technology, a CPAP (pronounced SEE-pap) machine.
"Our newest model," said Joan.
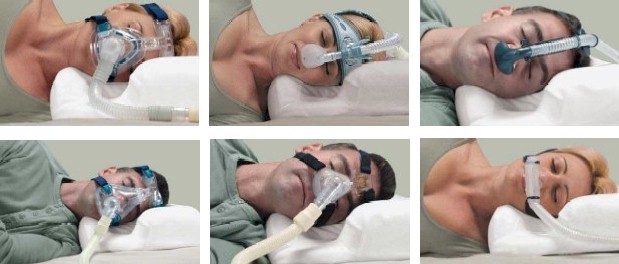
The machine itself was slightly larger than a lunchbox, a dark designer gray, with a corrugated hose that looped over my head and three slim black straps that held rubber nose plugs snug to my face.
"I gave you a medium," Joan said, looking critically at the nose plugs, which were now plugged into my nose. "If that doesn't work, you can try the large."
The large? I thought. I am not a large person. Is my nose really so out of proportion to my body?
But it was not the time to be vain.
Joan snapped on the machine. Oxygen flowed up the vacuum-cleaner hose on top of my head and through the nose plugs. When I opened my mouth, air came whooshing out, like I was some kind of human leaf blower.
"Don't open your mouth," Joan said.
I closed my mouth and nodded.
That afternoon, I took the machine home for a two-week trial. I hated the Darth Vader breathing sounds, the itchy nose plugs, sleeping with a hose on my head...but I used it diligently. If it worked, I was going to have to buy one—about $1,000. My insurance wasn't going to pay for it, so I had to be sure it was right for me.
After ten days, I caught one of the worst head colds I've ever had. I couldn't breathe through my nose at all, so I gave up on the machine. I was still sick when I brought it back to Joan.
"I don't think it helped," I said. I could see she was disappointed. We stared sadly at each other for a moment. I sneezed. She wrote me a referral to see a pulmonary doctor that afternoon.
The first question the pulmonary doctor asked was, "Are you sleepy during the day?"
"Tired? Yes. Sleepy...not really."
"Do you take naps?"
"I find it hard to nap," I sniffled. "I mean, I find it hard to sleep. Period."
"If you're not sleepy during the day, then you don't have sleep apnea."
"What about the sleep test?"
"There are different ways to interpret the results," she said. "But the breathing issue that came up, that could be from the sleeping pills you're taking. They depress the central nervous system. They could definitely cause shallow breathing. Especially if you've been taking them for a while."
"I've been taking them for ten months."
"That could do it."
"But it I don't take them, I can't sleep!"
"Yes, the antidepressants you're on can cause insomnia in some individuals."
We smiled at each other. Because the whole thing was so stupid.
"And on top of it all, I got this horrible cold," I said, because suddenly I was feeling really sorry for myself.
"Oh, yeah, I see that all the time," she said. "The CPAP can dry out your nasal passages and make you more likely to catch a virus."
Let's recap here:
1. Trying to work full time and raise young kids put my body under unendurable strain.
2. My body broke down.
3. The doctors decided that something was wrong with me, so they prescribed pills.
4. Those pills made it impossible to sleep, so they prescribed more pills.
5. The second pills depressed my breathing and made it look like I had sleep apnea.
6. The doctors gave me a machine to treat the sleep apnea, which dried out my (medium-to-large) nose and made me sick.
!
I called my doc and told her the whole story.
"In conclusion," I said, after pausing for a breath. "I don't think there's anything wrong with me. I just needed to quit my job, which I did. Now the only thing making me sick is the meds."
"There's a word for this," she said thoughtfully. "Iatrogenic. It means 'caused by the doctors.'"
Here's my diagnosis: It is crazy to put working parents in impossible situations where they are bound to go crazy, and then act like there's something wrong with them for going crazy.
Why am I telling you this story? Because there is a public health crisis afoot. We are suffering from a chronic state of busyness, particularly families with young children and two working parents.
We are also suffering from our adherence to a childish ideal of rugged individualism, which keeps us from supporting each other and from asking for help when we need it. This is not an individual pathology that can be solved with a pill (the effectiveness of which is now debatable) [1], but a massive cultural pathology that dictates everything from our individual relationships to laws and workplace policies that fail to support working families.
Make no mistake—at every step of this bizarre journey, I was in the hands of a competent and caring health care professional. They used every ingenious tool at their disposal to help me. The problem was, they didn't have the right tools. Where I needed work that challenged me without sucking the life out of me, they had anti-depressants. Where I needed someone besides my overworked husband to watch the kids for a Saturday, they had sleeping pills. Where I needed the support and encouragement of my peers, they had breathing machines.
So I'll leave you with this question: If our doctors can't help us, then who can?
Cross posted from the MomsRising column, A Peaceful Revolution, at the Huffington Post. A Peaceful Revolution is a blog about innovative ideas to strengthen America’s families through public policies, business practices, and cultural change. Done in collaboration with MomsRising.org, read a new post here each week.
Also cross-posted on Working Moms Break.
[1] NEWSWEEK, "The Depressing News about Antidepressants: Studies suggest that the popular drugs are no more effective than a placebo. In fact, they may be worse," by Sharon Begley, February 8, 2010



The views and opinions expressed in this post are those of the author(s) and do not necessarily reflect those of MomsRising.org.
MomsRising.org strongly encourages our readers to post comments in response to blog posts. We value diversity of opinions and perspectives. Our goals for this space are to be educational, thought-provoking, and respectful. So we actively moderate comments and we reserve the right to edit or remove comments that undermine these goals. Thanks!